August 13, 2020
Webinar: The Emotional & Physical Impact of Trauma & How to Heal
Written by Rachel Eddins
Posted in Trauma, Grief & Loss, Webinars and with tags: emotional trauma, trauma

You might be feeling overwhelmed due to some type of disturbing past event which shattered your sense of security.
This may have been some type of abuse, an accident, violence, a natural disaster, or another distressing event.
To help you make sense of the complex physical and emotional symptoms, the wellness talk will explore the after effects of trauma, triggers, and potential ways to heal.
Facilitated by Steven Serrano.
Watch a replay of the presentation here.
Learn more about our trauma and grief counseling services.
Here is a transcript of the webinar:
In today’s presentation, we’re going talk about some statistics for trauma, the difference between PTSD and complex PTSD, how the fight, flight, and freeze response works, how trauma impacts our physical, cognitive and emotional levels, and some of the potential things that we can all do to heal.
We will also have 15 minutes at the end of the session to answer any questions that you might have.
Learning Objectives
- Trauma statistics
- Difference between PTSD and C-PTSD
- Fight, Flight & Freeze response
- Impact of trauma (physical, cognitive, emotional)
- Ways to heal
- Q&A
Trauma Statistics
- About 60% of men and 50% of women experience at least one trauma event in their lives.
- About 7-8% of the population will have PTSD at some point in their lives.
- Of the cases reported to CPS, 65% relate to neglect, 18% to physical abuse, and 10% to sexual abuse.
- About 11-20% who served in Iraq have PTSD in a given year.
Source: US Department of Veteran Affairs, 2020
Let’s go with the statistics. As you can see here, statistics show that at least 50% of people experience some sort of trauma in their lives. And from those, somewhere between 7 to 8% have post-traumatic stress disorder.
An interesting percentage of children in people in the military also experience problems. So, for instance, as you can see, of the cases reported to CPS, 65% relate to neglect. There is 10% to sexual abuse and 18% related to physical abuse. Also, between 11 to 20% of people that go to war, like the war in Iraq, have PTSD in a given year.
I think an important thing here, is that when you think that there are people that don’t report, the percentages are probably even higher. There are some estimations in terms of sexual abuse, and rape, that people don’t necessarily go and report. As you can see here, trauma is definitely prevalent in our society. That’s the point I want to make here.
Difference Between PTSD and C-PTSD
Now we’re going to talk about the difference between PTSD and Complex PTSD. According to what we call the DSM-5, or the Diagnostic and Statistical Manual of Mental Disorders, for somebody to be diagnosed with PTSD, they basically have to be exposed to some traumatic event.
It can be related to death, for example, they were threatened to die. It can also be an actual threat or a serious injury or it can be related to sexual violence. These two things can happen if the person is experiencing PTSD. PTSD can also be secondary in the sense of a first responder, like a firefighter or a counselor that is hearing stories that are very traumatic, which can create also PTSD.
The other thing that I will mention is that in some of the folks in the mental health community, counselor therapies in general, including myself, we also believe that there are other one-time events that can be considered threatening and provide PTSD.
For instance, you imagine yourself as a wife that basically heard about her husband having an affair that can be extremely devastating and have PTSD-related consequences. So definitely there are other things that are not considered PTSD by the DSM, but they probably have similar characteristics.
Complex PTSD happens when people experience traumatic events for a significant amount of time without the possibility to run away from it.
A good example is to imagine a child that spends their first 10 years or 15 years, being abused by the mother or by the stepfather or, in situations where either the wife or husband had had some sort of violence. That can also be Complex PTSD.
When people go through very traumatic experiences, whether it is complex PTSD or PTSD and they can’t integrate, somehow the brain doesn’t process it. It leaves them with a feeling of emotions that results somehow in PTSD.
Here are some examples of PTSD and Complex PTSD:
PTSD
- Specific event(s)
- Accident
- Natural disaster
- Violence
- Death
- Secondary Trauma
Complex PTSD
- Prolonged exposure to trauma
- Emotional & physical abuse
- Sexual abuse
- Neglect
- Domestic Violence
Brain Integration
Left Side of the Brain
- Language
- Rational
- Present focus
- Based on facts
- Creates order
- Explains experiences
Right Side of the Brain
- Visual
- Spatial
- Intuitive
- Physical sensations
- Emotions
What we have normally is brain integration.
- The left side of the brain is the rational part. It’s about the present and it’s about creating a story that is cohesive, and about facts and statistics.
- The right side, on the other hand, is very emotional: visual, spatial, etc. It’s about basic human sensations.
For example, when we cry because somebody said something really sad, that’s the right side of the brain. It is very related to sound, touch, smell, and emotions.
Both the right and left sides of the brain work together, and they make meaning and experience.
So, for instance, imagine that somehow you’re on the streets and you smell your mother’s perfume while shopping. You may start thinking about her and how much you love her, the things that you talked about with her the last time you met, and maybe you start planning what are you going to do the next time you see her. This memory is also physical. You feel that nurture, and that warmth in your body when you think about your mother.
That’s why when some people say: “Oh, you’re much more right side if it’s the more emotional or left side of it’s much more rational.”
Let’s see what happens when there is any sort of danger. For example, you’re going to have a car accident. So when that happens, basically the left side of the brain is shut down. At that moment you are left with the right side, because at that moment, what we have to do is survive. We have to take an action.
There’s no time to think: “Oh, I wonder what is happening with that car. I wonder if that car is going to move”.
We do it automatically. We don’t even know when we do it because there is a part of us that takes action immediately. In a situation where there is any sort of danger and anybody goes through this, we make generalized conclusions, we take actions, and we don’t have rationality.
How the Brain Responds to Threats
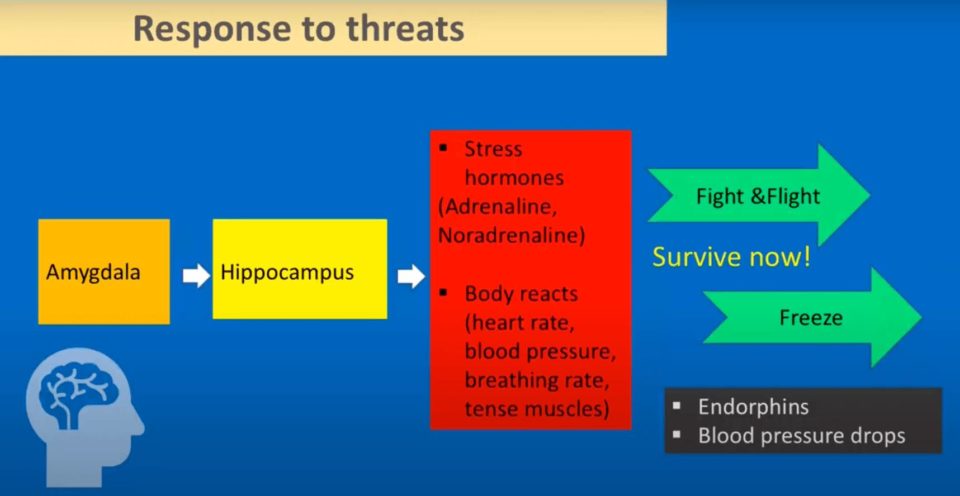
This is a very simplified version of other things that happen, so it’s not exactly how it is here, but it’s very easy to explain.
When there’s a threat, the Amygdala, which is basically the threat detector, sends an emergency to the body and gets help from the Hippocampus, which has some information on past experiences.
But then what happens when there’s an imminent danger?
What happens is the Amygdala says: “There is a real danger!” and it sends information that sends stress hormones.
- Those stress hormones provide the fuel needed to fight or flee.
- Immediately our heart rate goes up,
- We get high blood pressure, and
- We’re really there in terms of activity.
This is very automatic. We don’t sit there ourselves and say: “Oh, you know, there’s a danger, we’re going to do this…”
The other thing I want to mention that happens is, for example, let’s imagine that you’re in the wild and there’s a bear. What happens, is you can’t flee or fight for whatever reason So the system decides automatically that it is the time when we have to freeze. The first response is the freeze. It comes in and your body sends endorphins, which are almost like body painkillers. They’re like the Tylenol PMs of the body.
What it does is basically: “Ok, since you can’t do anything, I’m going to take up some of the pain just in case this bear is going to do something to you.” And what happens next is the blood pressure drops. What that does is avoid bleeding in case of an attack by the bear. So that’s what happens typically in any sort of danger.
Trauma is Personal
Before we start this conversation about what happens with trauma, I want to talk a little bit about the trauma itself. I want to say that trauma is very personal.
So when you think about the pain and the situations that you might be feeling, there’s something that you just can’t say which is that somebody has a bigger event than you, so they should be feeling double. Or, you can’t say that your event is bigger, too.
Trauma and everything we feel because of trauma is very personal and any event might feel big.
Trauma – A System in Continuous Threat
Let’s talk about why trauma is so complicated.
One of the most important things that happen with trauma is it makes people be very hypersensitive to perceive danger.
When I say perceive danger, what I mean is that sometimes danger can be there, but sometimes it’s not really there, but it seems like it is. That’s why it’s perceived danger.
When somebody has had some little trauma, danger seems really bigger than it really is.
This is because you’re exposed to so much information because of your previous trauma that it feels as if anything else is really, really difficult. And it is difficult because that’s what you’re feeling.
I think that’s an important point, that it makes it very difficult. Let’s use the analogy of the image above:
In this house, there’s an alarm that detects everything, including a butterfly outside. So, you know, after a while in this house, you don’t know if it is the butterfly or a burglar coming in. You start saying: “Well, I’m just going to stay awake, just to see if anything is going on.”
And that’s what happens with trauma. People are sensitive to what’s going on and past trauma can definitely be troubling and very exhausting for trauma survivors.
Another point that I want to make here is that we’re in the pandemic and we’re all together in this. So, you know, the pandemic has brought many triggers for everybody, trauma survivors and non-trauma survivors. Because obviously, we don’t know what’s going on, we don’t know if we can go out, and even going to a store might be difficult, everything feels very unsafe.
Using the analogy of the house, due to the pandemic the alarm sounds are probably even louder nowadays and even more continuous than before. For somebody that has already experienced trauma, the pandemic brings more triggers. And it’s very difficult because of that.
Symptoms of PTSD
- Fear/hypersensitivity to perceived danger
- Intrusive symptoms (nightmares, flashbacks, memories) as a way to integrate it
- Physiological distress
- Memory gaps & concentration issues
- Trust issues & less willingness to explore
- Anxiety/depression/anger
- Medical issues (immune system, sleep, headaches, pain, weight, etc.)
Now let’s talk about the symptoms of trauma.
One of the potential symptoms is intrusive symptoms (nightmares, flashbacks, memories). For instance, people that have some sort of trauma or PTSD have what we call flashbacks. Those are saddening and disturbing memories of past traumatic events. When people with PTSD are triggered it’s almost like they are there.
Let’s imagine that you were in the war, there was a bomb and people died. The people have sort of flashbacks or memories and it’s almost like they’re there. Their blood pressure goes up, and all the stress hormones go in. It’s really like it’s happening again, which creates a lot of stress for people that have survived some trauma.
Another point I want to make is that not all the symptoms, but these are some potential symptoms. The other thing I would say about when you have PTSD and a situation is happening again is that it’s sometimes very difficult to think rationally when you are triggered.
Somebody who has trauma might act without understanding the consequences sometimes.
Sometimes those intrusive symptoms are the way that the brain tries to heal itself. Precisely through those nightmares, flashbacks, and memories, the brain is saying: “Let’s work on this, I don’t like it.”
I heard somewhere in a presentation that the brain is kind of “lazy”. So the brain says: “We need to fix this situation” and that’s why it happens. Those sorts of flashbacks and memories can be really draining for people.
For people that have had trauma, it can take longer to balance themselves at normal levels. If you haven’t had any sort of trauma and you compare yourself with somebody who has trauma, balancing takes a bigger amount of energy and working more to be able to balance.
I have seen clients in sessions, and couples therapy is a good example, which have experienced trauma being constantly triggered and going into very difficult arguments. In such situations, it’s really difficult to notice that they’re being triggered by an old experience.
For instance, a traumatic event might feel similar to when the spouse is ignoring them. This feels like something similar that has happened before. But it’s very difficult sometimes to realize and make the link because at the moment you’re the trigger.
The continuous pumping of stress hormones in trauma survivors can impact memory.
Sometimes you have issues with attention. It is very difficult to pay attention to things or work. You can also see anger, or you can have issues with it. sleep. A diverse set of health issues happen.
- The immune system can be attacked if you are always being attacked by this sort of sensation that you are in danger.
- There are a lot of stress hormones happening. So that, of course, can work out the immune system.
- Headaches can also occur.
- I’ve also seen in the past that if people have had really bad trauma they feel pain.
The pain is real, it’s totally real but doctors can’t find what it is. It’s difficult, they don’t know what it is in some cases.
People that have trauma can confuse what happened in the past with what is happening today sometimes.
Because of that, sometimes new experiences might be stressful. When you are stressed by things happening, you don’t like the new things because they can be dangerous. That’s very much understandable.
Trauma can also smash the sense of trust and security that others provide.
If you have had a situation like past trauma, then you feel that it’s difficult to trust others. That can impact people in their relationships, and their intimacy.
For instance, if a child was abused by their parents, it’s difficult to trust others or if somebody has been raped, the area of intimacy can also be difficult. So, the intimacy area is also a part that can be can be impacted.
So there is like an alarm always going on, like running and running in your house. It creates anxiety, depression, and, like I said, many medical issues. As a therapist, I’ve seen some difficulties with people that have experienced trauma.
The other thing that I’ve seen is sometimes it’s difficult to recognize our emotions and our physical feelings. If you have always tried to be away from those feelings because they are really tough and remembering those sorts of feelings of past trauma, is not something that you want to do. So, it becomes a kind of normal life.
Sometimes it’s difficult to just say: “Oh what do you feel? What’s going on with you physically?”
Symptoms of C-PTSD
- Negative perception of self (shame, blame) & others
- Interpersonal sensitivity
- Longer time to recuperate than PTSD
Coping through:
- Avoidance (places, people, thinking about the trauma)
- Emotional numbness impacts interests
- Detachment & disassociation (emotions, body. mind) requires brain energy
- Self-medication to control exhausted system
Now, we’re going to talk about the symptoms that relate to complex PTSD. So let’s think a little bit about the example of a child that was abused by caregivers. Imagine that you are a child and you’re at home, and your parents are doing stuff to you that they shouldn’t do. They should keep you safe, and make you feel loved and nurtured. But that’s not happening. Well, what happens is the child, in order to survive, says to himself: “You know what, my parents or caregivers are good. It’s not their problem. It’s not them, it has to be me.”
People that I worked with in the past which have suffered sexual abuse or some sort of childhood abuse or neglect, have a sense of guilt and shame about themselves despite that they are the victim.
As a child, you learn that the people who are supposed to be taking care of you are not there for you. Well, you can’t internalize that because it will be devastating. So, the best way is to think it’s them. Sometimes, of course, that brings pain and loading.
These are things that are happening for longer periods, so complex PTSD can take longer time to work on than having PTSD.
You want to avoid that sort of pain that you’re having. Some people, as a coping mechanism, use avoidance. You know, maybe: “I don’t want to see those people. I don’t want to talk to people. It’s uncomfortable to be in crowds.”
For others, it might be substance abuse. Sometimes it’s just Facebook or Instagram, turning to social media to shut down. What they are doing there is disassociating from the pain. The other problem with that, too, is that if you’re when you try to let the pain go, and you don’t want to feel the pain. Sometimes the problem is that sometimes you lose the pleasure, the play, and the joy.
Harry: “I just feel so angry all the time… What if after everything I have been through, something is gone wrong inside me? What if I am becoming bad?”
Sirius: “I want you to listen to me carefully, Harry. You are not a bad person. You are a very good person who bad things have happened to.”
Source: Harry Potter and the Order of the Phoenix (Warner Brothers, 2007)
I really like this quote from one of the Harry Potter movies, because I think an important point is that trauma is not the person’s fault and it is done through a person.
Healing Trauma
Let’s talk about healing. The amount of work required to heal depends on the person and the situation that happen, but healing is possible. I’ve seen it in clients and they can do it.
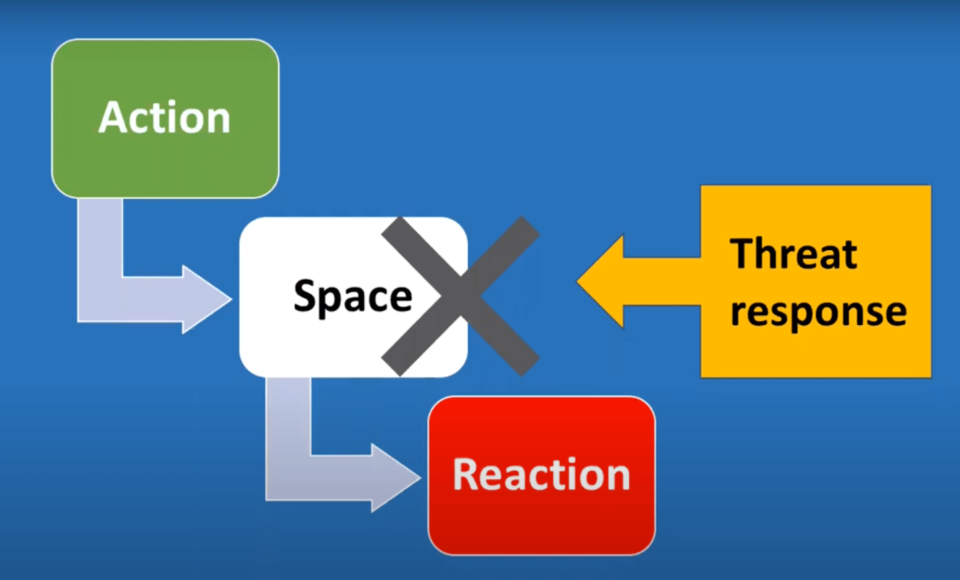
One of the most important things that are needed when we have experienced trauma is to find that space. What happens is we get triggered by an action and we feel it as a threat response. Somehow it triggers something in us and there’s a reaction. One of the things that are really important is to find that space. The space to say: “What do I really want to do here?” vs “I’m just going to react.”
Unfortunately, the reaction is unconscious because we got triggered.
One of the things that are really important is to be able to find that space where you could kind of relax. Because one thing that I do want to make very, very clear in this presentation is that trauma is physical.
I’m not saying that the traumatic experience has to be physical, but when we feel trauma, the area that we’re feeling is in the body. We feel anxiety, or we feel that pumping.
So, the door to healing starts with the body. That’s an important point that I would say here.
EMDR therapy and Brainspotting therapy can help you heal trauma stored in your body.
The idea of healing is not to forget those stories. Those stories are part of life.
The focus is to handle the emotions more separately. So avoiding negative impact. That’s what healing is.
Sometimes we don’t want to remember those moments, but we have to revisit them. But, of course, it’s very important that when we visit and we do it with a person, a therapist, group therapy, etc., we feel safe.
We want to do it. Nobody can pressure us to do that. That’s very important.
How To Heal Trauma
- Create a support network
- Finding meaning
- Mindfulness & meditation
- Yoga
- Breathing
- Self-soothing
- Journaling
- Healthy relationships with food
One of the things that are really important to healing is creating a network. When I say a network, it includes a lot of things here. It might be an individual therapist. It can also be trauma groups because these groups are a place where trauma experiences can be shared. Trauma groups are really therapeutic because those are places where experiences that we have had can be shared with others that had similar experiences. And that is really cathartic.
Having been able to talk about those things with others is really, really helpful. It’s important to find a group that feels safe.
For people that have substance abuse, the support network is, for instance, having a sponsor. The sponsor is there if there’s some sort of need, you can call them and that is really helpful. So that’s part of the support network.
Even pets are, from my perspective, a support network. This is because the pets provide safety and we feel totally loved by a pet. I think having pets is sometimes very important too.
The other thing is that as we tell a story on and on in the group, to the sponsor, or in individual therapy, it changes. We can tell it a hundred times and it feels different as we tell it. So that’s an important point.
Finding the meaning in the experience is also very supportive of healing because trauma has been done to people.
It hasn’t been done by themselves (in many cases). It has been done by other people, other situations or, maybe because of the pandemic itself.
I have worked in the past with trauma survivors that suffered sexual abuse from the parents themselves and it’s devastating. Because of that situation, there were relationship issues, anxiety, depression, and even weight gain. There is always that feeling where you want to put something between you and the other person.
Through the process of therapy, she was able to explore her trauma, find peace, and encroach on some sort of meaningful experience which was vital for the work of trauma from my perspective.
This person had an incredible, incredible story from my perspective, and that was one of my first cases as a therapist.
She learned through the process to find some sort of empathy for people with similar experiences. And she wanted to help people.
It was about: “How can I do something for somebody else?” That’s really important in the process of healing.
I always tell my clients: “Meditation, meditation, meditation!” I say this because mindfulness and meditations are incredibly helpful for anyone whether they going through trauma or not.
There are studies out there that have shown that people suffering from depression, anxiety, and chronic pain, have benefited from regular meditation and training.
There are also studies that say it helps the immune system. It can help with blood pressure, and emotional regulation, and it can help people react less.
So I’m a 150% fan of meditation and mindfulness. Mindfulness techniques can also help trauma survivors focus on their emotions.
As I said before, sometimes people who have trauma have difficulties seeing what they feel.
So by sitting down, it’s incredible to be able to say: “For the first time I can see what’s going on with me.”
It also soothes the nervous system. And because of that, it avoids going into a fight, flight, or freeze response.
The other thing that mindfulness does is helps to activate the prefrontal cortex. That’s really good because then we can think: “Is this good or bad?”
Because if we have rational decisions is much easier to see. “What is my action? And if I do this, what are going to be the consequences in this relationship with this situation?”
The other one that I’m a super fan of is yoga. I really wish I could do more yoga. The pandemic is not helping, but I found very good yoga exercises on YouTube. There are tons of videos.
Yoga practices can improve cognitive functions. It can help with your mood and it can help with stress coping.
Yoga also has excellent benefits in the area of PTSD because it decreases the activity of the amygdala and the stress response.
One of the points that I want you to take with you is that many of our emotions are linked to body sensations. We don’t necessarily think about it because we’re depressed or sad or mad, we think it’s in our brains. But if you go to your body, it’s really there.
I’ve heard from people that I worked with that fear is coming through the stomach. When you start understanding the physical situations, you focus on them, you calm the physical feeling, and this time the emotion. The idea is to go from continuous energy to feeling safe. So the body, from my perspective, is the door to healing.
Breathing is another really important way to heal. It’s a way to calm the mind and the body. Another thing that I really like when people do, it’s writing about trauma. It’s sitting down and putting that experience outside of you and seeing it outside of you. It’s extremely important because then you can go as slow as you want to, you can be in the moment, and you can decide not to write more. You can decide to cry by yourself. Whatever works for your trauma integration.
The other thing I would say is a healthy relationship with food. For some people, it might be eating too much, for others eating very little. Both are bad. There are studies that talk about probiotics. They still need to do more research, but they have noted how those probiotics are a link between other things like mental health, depression, etc. The relationship we have with food is extremely important because that tells the story of what’s going on with us.
Mindfulness Exercise
I want to do a little mindfulness exercise. I don’t know where you are, but if you’re with people and you feel unsafe, you can not close your eyes. And if you feel that you’re in a good place, I want you to close your eyes. As you close your eyes, I want you to sense your body. And as you sense your body, I want you to take a breath that is really deep. Breathe deep in, and as you let go, I want you to say to yourself to relax.
I want you to breathe in, breath out, and stay relaxed. Let’s do it again. I want you to breathe in, breathe out, and relax. As you stay in this sort of feeling, I want you to handle that sensation of breathing. Maybe the air is coming in and it’s kind of cold and leaving your body, which is warm. I want you to just focus on that breathing for a second.
Maybe as you focus on breathing, you just focus on the sensation in your body. Maybe you have something in your back that feels painful, a tension, or maybe your legs because you went running today. Whatever it is, just be with that sensation. I want you to focus on really letting that tension go. And those sensations, let go.
Scan Your Body
As you feel that, I want you to scan your body again. Notice the difference. The next thing I wanted to do is, if you have any sort of tension in your body, imagine that you just let it go. It’s almost like a river passes through your body and you just level the sensation. You relax and you feel that. You see the importance.
Maybe they were a thousand things on your mind today. There were things you had to do, and you did or didn’t do. At this moment, they really matter. Even if it’s just a small station or relaxation, maybe you felt that. Even if it’s minimal, it’s ok. And that’s why I think it’s important finding that space and do all the things that we discussed.
EMDR
- Phase 1: History and Treatment Planning
- Phase 2: relationships, education, relaxation techniques
- Phase 3: Assessment – target and measure target (negative/positive belief)
- Phase 4: Desensitization – work on the target
- Phase 5: Installation of positive cognition
- Phase 6: Body Scan to review residual tension
- Phase 7: Closure of the session – explain what to expect
- Phase 8: Reevaluation of the situation and treatment plan
Work with an EMDR therapist to heal from trauma.
(www.EMDRIA.org, 2020)
Reading Suggestions
- “The Body Keeps the Score” by Bessel van der Kolk MD
- “Walking the Tiger – Healing Trauma” by Peter Levine
- “Trauma and Recovery” by Judith Herman
- “Journey Through Trauma” by Gretchen Schmelzer
- “The Journey from Abandonment to Healing” by Susan Anderson
- “Adult Children of Emotionally Immature Parents” by Lindsay Gibson
- “Complex PTSD: From Surviving to Thriving: A Guide and Map for Recovering from Childhood Trauma” by Pete Walker
- “The Complex PTSD Workbook: A Mind-Body Approach to Regaining Emotional Control and Becoming Whole” by Arielle Schwartz
These are some of the books that I really like. If I’m a fan of the first one, “The Body Keeps the Score” by Bessel van der Kolk MD. He talks a lot about some of the stuff we talked about today. He talks about the impact of trauma and explains in more detail some of the potential ways to heal.
The second one, “Walking the Tiger – Healing Trauma” by Peter Levine talks about the role a body plays in trauma.
The third one, “Trauma and Recovery” by Judith Herman describes what happens with the different sort of trauma that exists and the stages of recovery anyway.
Bibliography
- Van der Kolk (2015). “The Body Keeps the Score”. Penguin Group
- Herman, J. (2015). “Trauma and Recovery: The Aftermath of Violence – From Domestic Abuse to Political Terror”. Basic Books
- Breit, S., 1, Kupferberg, A., Rogler, G., Hasler, G. (2018). Vagus Nerve as Modulator of the Brain-Gut Axis in Psychiatric and Inflammatory Disorders
Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5859128/
- Jennings, A. (2004). The damaging consequences of violence and trauma: Facts, discussion points, and recommendation for the behavioral health system
Retrieved from: http://www.theannainstitute.org/Damaging%20Consequences.pdf
- The U.S. Department of Veteran Affairs (2020). National Center for PTSD – Understand PTSD.
Retrieved from https://www.ptsd.va.gov/understand/common/common_adults.asp
This is the bibliography and some other things that are worth mentioning.
Questions
How is self-soothing different from breathing?
I think that when we breathe, we self-soothe, but we can self-soothe in many other ways. Being able to breathe just by itself is another fantastic one to relax. The other one that I really like is the one called 4-7-8. Basically, you breathe in, count to 4 and wait there until you count to 7 and you let go to 8.
I would say that you can self-soothe in many ways. I, for instance, with the pandemic and everything stressful going on, chose walking. I walk for 45-60 minutes and I put on this very relaxing music. Sometimes, because I am a Hispanic person I put salsa.
So that’s my way to self-soothe. For somebody else. it might be running or painting. There are different ways we can self-soothe from my perspective. A really important thing is to look for ways to relax your body. Being able to exercise is a very good way, but so is sitting down for 10 seconds.
What is the connection between tinnitus and trauma?
I don’t have a huge amount of experience in that area, but I do know from reading that PTSD sometimes increases tinnitus. When you think about the number of stress hormones and high blood pressure, you can see there’s a connection there with tinnitus.
I think that there is a bunch of different things, including pain. Some folks feel pain. I’ve had people working with me who have gone through tens of doctors and they can find the cause of the pain. So there are several things, including tinnitus that might be related to that.
Can you choose the right response if you know what your emotional triggers are and you are triggered in a certain situation? I know that our body automatically reacts based on the fight, flight, or freeze, but is actually choosing the right response so you can soothe yourself within that situation?
There are different ways of dealing. So, for instance, cognitive behavioral therapy works with the thought process. The thought process includes working on your thoughts so you don’t get triggered or if you get triggered how to get out of that trigger. It can be thought-related from our perspective sometimes.
EMDR therapy works too. Let’s imagine that you have had this horrible accident and you can never go on highways because you get triggered. The EMDR works on those emotions because what we lost is the connection between the emotion and the rational part (it is more complicated than that but to make it simple). We’re left with the emotions and the feelings and EMDR works on these emotions through a process.
The other way that you can do that is through relaxation of the body. That’s one of my favorite ones because if we relax our bodies, we are calmer. I had a person that came to me and had a huge amount of anxiety and started to work on meditation. He started to calm down and it was easier to for him react in the office.
The bottom line is that there are different ways that you can basically learn to soothe or not get triggered. They’re all good, different ones. Some people don’t like cognitive behavior, some people do. So it’s very much dependent. Different tools can help.
Comment from a participant:
For example, you have suffered from childhood bullying and now you’re in college. When you are around your peers, you feel social anxiety because you don’t feel safe at that moment. Would you recommend flight and leave or would you recommend flight and stay in the situation so you can get through that social anxiety and be able to interact? Or would you just recommend freezing until everybody leaves you alone? Which is the best response because your body is going to react?
What we need to work on is decreasing that reaction. So if you have been feeling some sort of reaction because the person present was a bully, you need to work with those sorts of feelings that come from the bullying. Being able to say: “How can you calm yourself?” You call this reaction a “fight”, but I call it exposure more than a fight. I don’t think fighting is good in any case. In terms of “flight”, sometimes we have to do it.
Can we start exposing the person slowly to these feelings? I think the bottom line is we have to work on the origin and the origin is bullying. It’s important to work on the origin because if you’re going to fight you’re always going to be reacting and that’s not helpful. So you can implement EMDR, exposure therapy, and other things.
Have you personally had experience with trauma?
Yes, I have. I have had experience with personal trauma, and different things that happened to me all my life. That’s why I really like to work with people that had trauma. I guess there was some empathy in the sense that I’ve had situations that have happened to me and that I have been able to work through them. I really want to be able to help other people to do the same sort of thing.
Would you say that the physical healing or coping methods such as yoga, and breathing, are more effective than the mental, and emotional ones such as finding meaning, or understanding from others with similar trauma?
I think it is very personal. I do EMDR, and some people love it and they say this is the best thing in the world. And some people don’t want to do it. From my perspective, the first thing that we have to do when we are working with the body is to really relax. That’s very important.
We also need to do other things, talk about the trauma, as well as connect the trauma and integrate it. But from my perspective, we have to use a bunch of tools. I mean, for example with the case of the pandemic, I needed to feel that I’m able to sit down after a full day of talking to people.
The tools I use work for me, but maybe they will not work for somebody. I don’t think that only sitting with some coping methods can be very helpful. In some cases, any sort of therapy is needed. For some people is couples therapy, as a matter of fact, working on the trauma together.
Is going to sleep a way of relaxing the body?
Yes, if you sleep well. The problem is some people don’t necessarily sleep well. I’ve heard that sometimes having a nap can change the way you think about things. So not from the mental health perspective, I think that sleep can be really important. If you don’t sleep well and you have horrible nightmares every day, you’re not going to be able to function.
Which one do you have PTSD or Complex PTSD?
I will basically say more Complex PTSD because of situations that happened to me when I was a very young person and the impact that they had on me. I’ve had experiences with people that have PTSD or Complex PTSD and sometimes both of them.
How do you help people isolate the trauma that has been blocked for so many years? Do you need to completely identify the triggers before going through them?
I’m going to give you an example where that is not necessary. You can work with EMDR on some of the things we don’t necessarily talk much about. You don’t need to tell the therapist a bunch of stuff. That’s an example where sometimes it’s not necessarily needed.
It’s really important to be able to find ways to soothe yourself before you start telling the story because otherwise, it can be very traumatizing.
If you’re super anxious about telling the story, you have to learn to be able to relax. You don’t have to go to a therapist and tell this story immediately. You can just go slowly and get to a point you feel comfortable because it’s important to trust the person you’re talking to. And then as you work, you can start looking at some triggers that you never thought were related to that trauma.
Thank you very much for being with me here tonight. I really hope that this was helpful.
We have a bunch of people in Eddings Counseling Group that work with different types of traumas. There are all sorts of people you can reach out to. You can have a 15- minute consultation if you don’t have a trauma therapist and see which one you like best. And hopefully, this was good for you and it was helpful.
Have a great night. Take care of yourselves. Be safe and think about how can you really find ways to self-soothe. Thank you very much.