March 11, 2021
Webinar: What You Eat Affects How You Feel (and Vice Versa!)
Written by Rachel Eddins
Posted in Emotional Eating & Body Image, Webinars and with tags: Emotional Eating, Food, Food and Body Image, Make Peace with Food

Our relationship with food is complex and unique to each of us.
In this webinar, we explore some of the ways in which nutrition and mental health are intertwined, and which core principles may guide us towards improving both.
Facilitated by Heidi Hoarau, LPC- Associate.
Watch a replay of the presentation here.
Learn more about the connection between nutrition and mental health.
Here is a transcript of the presentation:
Hi and welcome to this webinar on the connection between what we eat and how we feel and on how to use nutrition to feel better. I am Heidi Hoarau, a therapist and a health coach at Eddins Counseling Group. I’m really excited to share this topic with you today.
The topic of nutrition and mental health is really dear to my heart. First, I think that food is medicine and also because I think it’s key in terms of helping recover from stress and trauma. As a therapist, I specialize in helping people heal from trauma.
So that’s a topic that it’s very important to me. Let’s get started.
Nutrition and Mental Health
- Understanding the interplay
- Through personal experience
- From the latest research
- Improving mental health through nutrition
- Through food
- Beyond food
Here’s what we’re going to go through today. So we are going to have two parts.
In the first part, we’re going to get curious about really understanding the connection between body and mind and food and mood.
We’re going to try to understand it first through our personal experiences with it, and then look into research and what we can learn about the biological mechanisms that are involved in that connection.
That’s really in the logic of understanding more of what’s going on. Have an appreciation of what’s involved and from that understanding, I guess, being more appreciative and kind to our bodies and to our relationship with food as well.
The second part would be about how to improve mental health through food. We’re going to talk a little bit about beyond food as well.
And then, in the end, I’m going to share some of the references and opportunities to get support, if you are interested to continue that conversation and that exploration after watching that presentation.
The first part is to really look at how we experience this mind-body connection.
We’re going to start with the connection from our mind to our body. We’re going to do a little bit of an experiment and guided imagery to explore what happens when we think of something and how it may affect our bodies.
The Imagery Exercise
The experiment: I’m inviting you to do the “imagery exercise”. I’m going to walk you through it and see if you feel anything. I’m going to ask you to sit comfortably and take a few deep breaths right now. When you’re ready, close your eyes or lower your gaze and start imagining that you’re standing in the kitchen (whether it’s yours or a kitchen that you have good memories from).
Just take some time to imagine which kitchen you would want to visualize right now.
When you have chosen one, just settle with that one. Imagine that you’re entering this kitchen and start glancing. As your gaze gets close to the counter, you see a beautiful wooden cutting board there. And on that cutting board sits a bright yellow lemon, and you can start noticing its color, size, and shape.
You reach up, pick it up, and notice how it feels on your touch. Maybe it is smooth or bumpy, maybe you’re touching the end where it was attached to the tree.
Just take time to see what shape it is and how it feels on your hand.
Next to the cutting board, you see a sharp knife. I encourage you to look back at the cutting board and pick up the knife. Then, with a steady hand cut the lemon in half.
As you do this, you see the knife slicing through the fruit, the fruit will open and reveal itself. Maybe there are seeds inside and maybe some drops of juice will spill.
Now take half of the lemon, cut it again, and get a quarter slice. After you put the knife down, just bring it up to your nose.
Make yourself aware of the citrus scent and smell.
Then you bring the lemon to your lips and just notice the sensations. And then you can open your mouth and actually bite the lemon. Whenever you’re ready, you can open your eyes again and get back to the presentation.
Some people have actual physical sensations just based on imagining that scene and that speaks to the key the mind plays in imagining something.
Sometimes it feels as real as actually living it and the body reacts the same way. So that illustrates the mind-body connection.
Another way you can also use it for yourself is to see how you react to mental stress.
- Some people may feel the tension in their bodies, their jaw, neck, shoulders, or back.
- Some people may feel it in their head (more headaches, dizziness), in their heart (heart racing or chest pain, shakiness).
- Some people see it as digestion issues.
And that’s an important one that we’re going to see and revisit.
We’re going to understand the link between stress and digestion as well. That’s a way to notice how our mind is influenced by our actions.
Let’s go now from both directions, from the body to the mind.
For that one, you can remember what you feel when you’ve been drinking a caffeinated drink, for example.
Some people feel energized or focused, some feel actually calmer or sleepy, some feel agitated, wired, or anxious, and some people don’t feel much after drinking a caffeinated drink.
So whatever is right for you, that’s the kind of thing that can indicate that what we drink affects our mind.
This is the same as when you eat your favorite food, and what goes on in your mind after that.
You may feel some pleasing sensations, good memories coming up, or just a good feeling. That’s a way in which we realize that connection from the body to the mind as well.
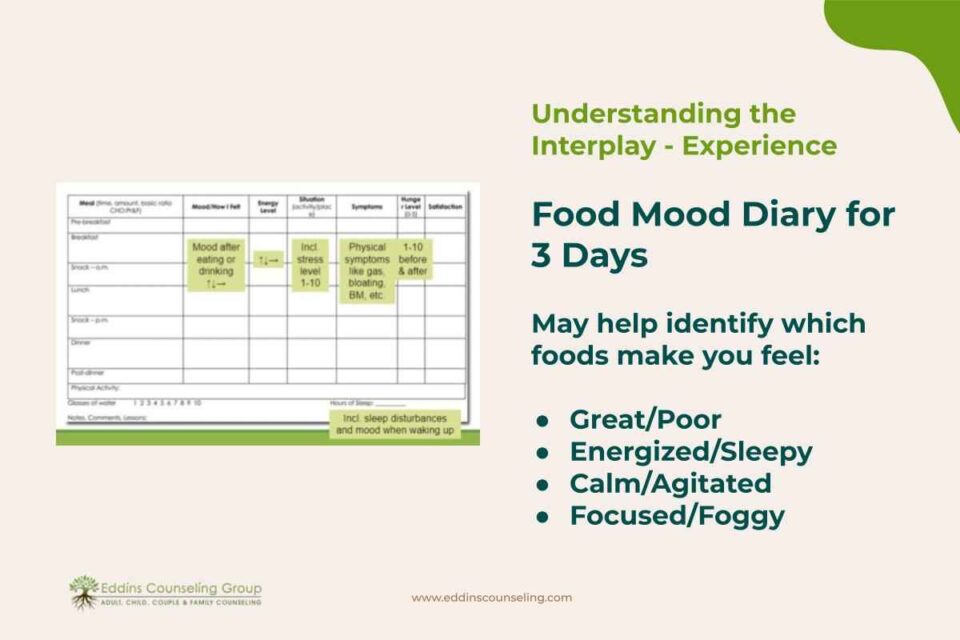
To understand that connection a little bit more (because sometimes it’s not clear what the influence of what we eat is on how we feel), doing an exercise in the Food-Mood Diary can help us notice and pay more attention to what we eat and how it affects how we feel.
That’s a lot of different variations of the Food-Mood Dairy on the internet so pick one that suits you. But I think that one where you indicate what you ate in the first column and put the time of both the drinking and the eating and what you ingested. And then in the other columns, you indicate how you felt right after that.
- Was it the same mood?
- Was it better or worse?
- What about your energy level?
- Did you feel more energized, less, or the same?
- How did you eat or drink?
- Where were you?
- With whom were you?
- What was your stress level? Maybe using a scale of one to 10?
- Did you experience any symptoms after that? Physical symptoms like gas, bloating, etc.
- What was your hunger level before and after?
And we’re going to talk more about the scale as well. What was your satisfaction with that drink or meal? You can go through that throughout your day and you don’t have to do it for too many days.
Three days is usually enough to give you the idea of a pattern of what food does to your mood.
And you can indicate as well if you’ve done any physical activity that day, how many glasses of water did you have, how many hours of sleep you got, and if the night after that day was disturbed and what was your mood right after when you woke up?
Do you think that this exercise can actually give us a lot of information and make us more aware of what food makes you feel great, poor, or focused after you eat all of these things?
Another thing that is important to become more aware of is what are our signs of physical hunger and distinguishing when it’s actual physical or emotional hunger. Signs of physical hunger would be more like a growling stomach or sense of stomach being empty, maybe feeling connected or having a headache, feeling irritable or shaky. So those would be signs of physical hunger.
Emotional hunger could be more like fatigue and sometimes we are confusing hunger and thirst.
So I actually may be thirsty. When it’s emotional hunger, maybe what you need is actually a break. Maybe you’re feeling exhausted, or fatigued, and you need a break or you need to move or you need to connect with someone. So these are signs of different needs that may not actually be hunger.
If it is hunger and you are aware of where you are on the scale, that can be quite useful with the 1- being so hungry that you don’t know anything about and 10-that you’re actually I’ve been eating too much and you feel actually uncomfortable and even maybe in pain.
And what you would want is really ideally to stay within the 4-7 range, which means that you would eat when you just feel a little hungry.
So when feeling the first signs of physical hunger but not drastic, where you have to act on it right away. This way you can have time to prepare, sit down, and stop when you’re completely satisfied.
That may not be 100% full. It’s actually pretty close to 70% full. So that’s maybe something that we’re not used to doing. That may mean eating more regularly every few hours, for example. But that’s not a program and we’re going to see that way afterward as well.
But what is more of a problem is if we actually wait too long.
When we restrict too much that stresses the body, it gets a signal that food is scarce and so it brings up all of us mechanisms of first alerting you that you’re really hungry and making you really increase that appetite and make you crave eating.
And then it also kind of changes your metabolism, because it says: “Ok, well, everybody needs to slow down because I’m not having as much energy as I actually need. So let’s slow down all those things that are not essential and could be productive, for example, storing energy resources and consuming it, because we are not sure when the food is going to come.”
It’s important to restrict food and not eat as soon as we’re getting hungry.
Now we’ve gone into the personal experience of that connection between the body and mind, and let’s see what we can learn from the research.
As I said, this is really just to get more understanding of what’s actually involved and get more precision from it. Hopefully, I will find a middle ground where it’s not too complicated or too simplified, but gives you a good view of the mechanisms involved or what is what we know of them because that’s really something that is still being researched. So we don’t know everything about it. But I want to share what we know or at least some of what we know. It’s not going to be exhaustive, of course.
We’re going to start with a high-level review of the body and then we’re going to dig down more into the intestines. We’re going to zoom in little by little.
The first picture is the body from the brain to the intestines. The first system that it’s available there is what we call the Central Nervous System, that’s comprised of the brain and the spinal cord. That’s what we call the First Brain.
Then, we also have another nervous system, which is called the Autonomic Nervous System. That one has three subsystems. We are usually knowledgeable about the Sympathetic and the Parasympathetic, and a little less about the Enteric Nervous System.
I’m going to present a few of them.
The Sympathetic Nervous System is the one that allows us to react to stress and get us ready to fight or flight.
It activates muscles and gives us energy. This is including a Sympathetic Ganglia system that is going along the spine.
Then the Parasympathetic nervous system kind of does the opposite.
It’s actually the one that is involved in the relaxation response after stress, and that one involves what we call the vagal nerve. That’s the red nerve that goes from the top of the spine to a lot of organs and especially the stomach and the intestines. We’re going to see that in our pictures as well. It is a very important one. That means that the relaxation system that we have is actually involving the stomach and intestines.
The last system that I mentioned is the Enteric Nervous System, which is the one that is actually within the gastrointestinal tract or the gut.
Those are all the nerves that are actually present in the stomach and the intestines or the tract. And that’s what we call the Second Brain.
This is another system that is not nervous. So it’s not a system of nerves and neurons, that can cause the neurotransmitters, and allows communication between the neurons. But it’s also of systems that we have, which is a chemical one. So it’s the hormones, etc. and that’s what we call the Endocrine System.
We have a lot of endocrine systems, like the thyroid. But the one I wanted to illustrate here, as well, is the HPA axis, which is the one that is involved in the central stress response. Just for you to visualize where those organs are, it involves the Hypothalamic-Pituitary, which is in the brain, and the Adrenals we’re going to mention the time in the presentation which are sitting on top, that’s just above the kidneys.
This is how it works: when we have stress, it sends a signal to the Hypothalamus, which sends the Pituitary gland, which releases chemicals that the Adrenals are going to see and release the first alarm chemicals, which are the adrenaline and noradrenaline.
The one that takes a bit longer to get released is cortisol. Cortisol releases signs that we are good, we’ve done our job, and there’s enough cortisol in there. Now you can inhibit the signal and get back to normal, baseline level.
When there’s chronic stress, that feedback loop doesn’t happen. It gets dysregulated and the cortisol level actually stays high in the blood all the time and that creates a lot of damage to the body.
Another thing that happens when that cortisol is released is that it’s reorganizing the priorities and it puts everything forward positively towards the fight or flight response, but it shuts off or reduces the odds of systems like actually the cortex that makes us think, plan, see the consequences of what we do. That tends to work less.
Also, the other systems like digestion and the immune system kind of get onto the second priority as well. There aren’t many resources so they don’t function as well.
Link Between the Brain and Guts
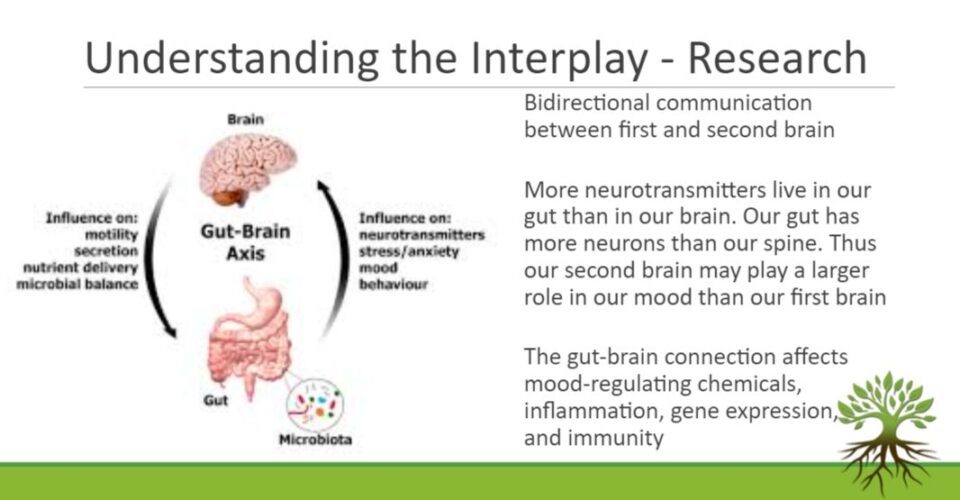
Another illustration of the link between the brain and guts. This link involves bidirectional communication, the same as the connection of the brain with the body.
It illustrates what is going on in that one way and another away. So I think to know is that actually, in itself, more neurotransmitters living in our guts than in our brain, because that’s actually where they’re getting produced (most of them), and that the guts actually have more neurons than our spine.
It’s just really a lot of the same infrastructure as the brain. It has nerves, neurons, and neurotransmitters. In a sense, it’s it may have an even larger role to play in the mood.
So that’s why you see that there’s a big direction between the brain and the gut where it influences the nutrients that are getting because we decide what we eat.
So our brain has an impact on what nutrients get delivered.
Stress has an impact on the microbiota in our guts because that can really affect the balance between good bacteria and bad bacteria.
The other way between the guts and the brain is the neurotransmitters because most of them are produced there and then get released into the brain. If we don’t have the right nutrients to be able to produce the neurotransmitters, then they don’t get produced in the right amounts and that can create imbalances and affect us.
We need a good brain connection from regulating chemicals, which are neurotransmitters but also influence inflammation levels.
So gene expression, because what our cells inside see in terms of nutrients, toxins, chemicals, and levels of stress affects which genes are turned on. Immunity is also well connected because it is actually sitting in the distance. So it does get involved here.
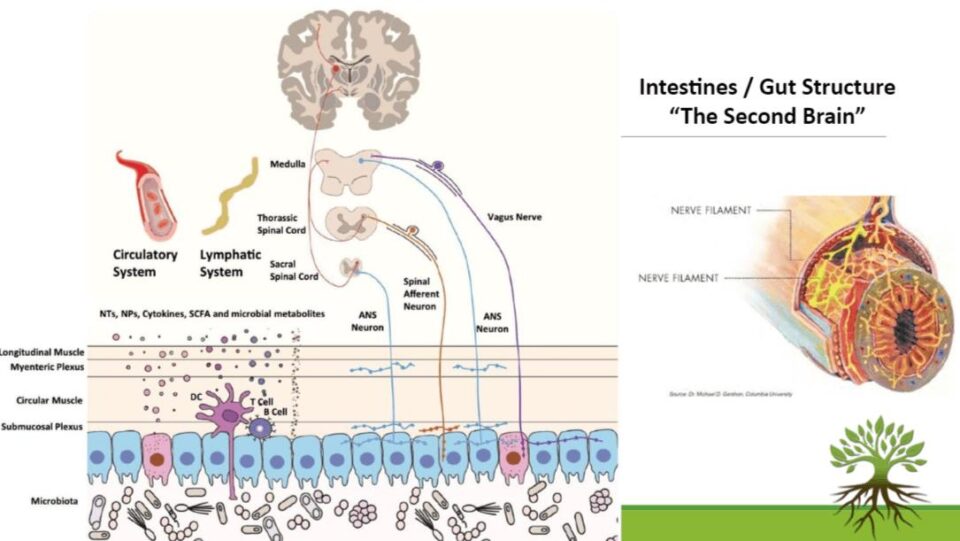
Here we see the brain at the top and the three levels of the spinal cord. Then, the bottom part is the intestines or cut of intestines where you see the top layers with muscles and then the inner membrane, which are cells that are in contact with the bacteria inside the intestines and microbiota.
On the right, you have a picture of a cut of the intestine, and that’s where you see where the nerves are located. All the little parts are actually nerves. So those intestines have a lot of those.
In the picture on the left, you see the bigger nerve again that connects the top of the spine or the brain to this little pink cell here, and we’re going to discuss that in the next slide.
What you see here is also the immune system being so close to the digestion system because those cells are the immune system and actually over 70% of our immune system lives in our gut.
It’s very interesting to see that’s all connected as well.
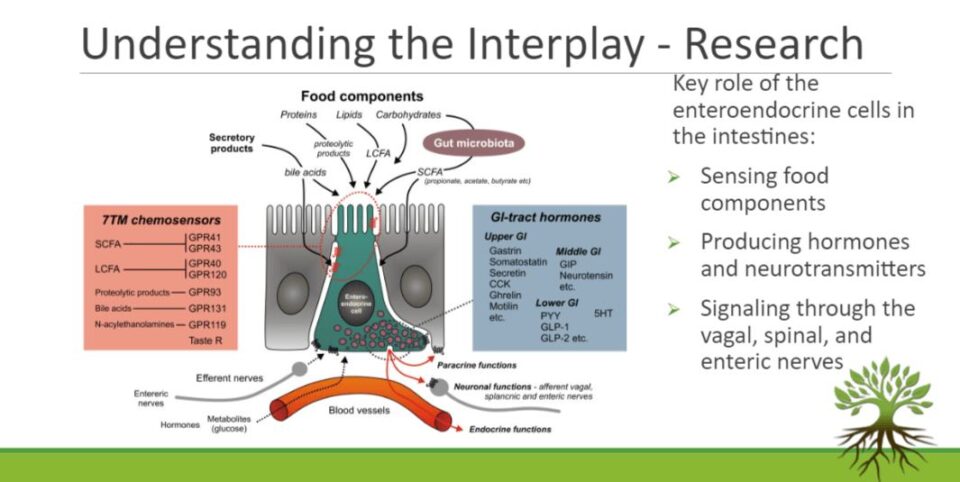
Key Role of the Enteroendocrine Cells in the Intestines
What about these little pink cells that we’re seeing in the membrane of the intestines, called the enteroendocrine cells?
What is really interesting about them is that they both sorts of have a key role in sensing the food components that are arriving inside the intestines.
That’s what we see at the top, the food components of protein, lipids, and carbohydrates. They are in contact with the good microbiota which are the living organisms that help us break down nutrients, transform food into nutrients, and create SCFA which are the short-chain fatty acids.
Those cells are sensing and they are the ones both producing hormones and neurotransmitters and releasing the hormones and neurotransmitters into the blood vessels.
They’re also in contact with the nerves. They both have a key role to play in the endocrine system. So all the chemicals in the nervous system, whether they go to the spinal and sensory nerves, аre connected to both.
We’re done with the more biological understanding. We need to understand mechanisms are complex and we don’t know everything about them yet. It’s still being heavily researched.
Nutrition is also a young science and there’s a lot that we don’t know yet about the effect of certain food on the body and individual reactions to them. But there’s quite a lot that we know as well.
So it’s a very interesting time when we start to understand all of that. We see lots of different factors and different factors of separate pathways to improve how we heal as well.
Improving Mental Health – Through Food
Some words of caution
There is no one diet right for everyone. Listen to your body!
These are guiding principles – some may not apply to you if you have specific conditions (e.g. food sensitivities, or thyroid issues – cruciferous vegetables to be avoided then)
Nutrition is closely tied to our identity (personal, familial, cultural, spiritual) and may also be associated with difficult experiences
- Acknowledge potential emotions that may arise from these topics (e.g. overwhelm, confusion, shame, anger, etc.)
- Be compassionate with yourself
That’s what we’re going to get into now and see what we can do to improve mental health through food. I want to kind of pause here a little bit, because we’re going to get into that section where I might say “do this” or “do that”. And I know that these discussions can be a little bit triggering. So I want to kind of put some guidelines there first.
There’s no one diet that is right for everyone.
There’s a wide range of diets that are healthy that can support a healthy mental state. So there’s no one that is right for everyone. So listen, for your body, and for your individuality as well.
For example, maybe you have specific conditions, like:
- Food sensitivities that make you more sensitive to gluten or dairy or eggs or whatever. Being sensitive to that obviously is very important.
- Or maybe you have specific medical conditions like thyroid issues.
- Or cruciferous vegetables need to be avoided if you had kidney implants.
These are all individual situations that you need to be aware of and that means listening to what your body has to say as well. These are just guiding principles.
Don’t feel that you need to try everything and everything’s going to be good for you. I encourage you to experiment with them.
But obviously, if that doesn’t feel right, then it doesn’t feel right. And also recognizing that nutrition is closely tied to our identities or personal, familial, cultural, or spiritual.
There’s a link between what we eat and our sense of identity. It may also be associated with your expenses.
So it’s important to acknowledge whatever emotion is coming up when we’re talking about that. Acknowledge some words, some confusion, or emotions like shame or anger and recognize that that’s the first important part and that sense of self-compassion there.
Realize that you are already doing your best. You are enough that whatever eating habits you may not be happy about are not defining you as a person.
Remind yourself of that and bring less judgment and just more curiosity into the topic and see how that shifts your relation to what we say.
We’re going to go through all the nutrients that we are getting through food and we are going to explore in which way they are all important and then say a few things about each and things that are better or worse.
FATS
- Provide energy and lubrication for the brain
- Are essential for the absorption of nutrients and fat-soluble vitamins (A, D, E & K)
- Provide essential fatty acids (omega-3, omega-6, and arachidonic acid AA) – essential for neurotransmitters to flow and for cell membranes
- Any type is fine (fishes, avocados, nuts, seeds, oils, even saturated ones), except for trans-fat, “hydrogenated”, “partially hydrogenated”, margarine, or shortenings
The first one is Fats, and they usually have a bad press. We’re going to kind of demystify that a little bit and hopefully, you can deconstruct any myths that you may have there. Fats are very important because the brain is made up of 60% fat, which is called DHA.
It’s the fat we eat to provide energy and lubrication for the brain. It’s also essential because some nutrients and vitamins are absorbed through fats and are just fat soluble. So if we don’t have the fat, then we’re not going to be able to absorb those nutrients or to actually absorb those vitamins like A, D, E, and K.
The fact that we eat fats provides essential fatty acids (omega-3, omega-6, and arachidonic acid AA) and those are essential for neurotransmitters to flow and for cell membranes.
In terms of what it’s to avoid or not, any type of fat is fine. Even the saturated ones that had bad press are not to be avoided at all costs. We actually need saturated fats.
What may have been worrying at some point is that through animal products we tend to get more saturated fat than we need. That’s maybe why there’s been kind of a push to be careful about the saturated ones.
Getting them from different sources so that we don’t get too much of them. Like, for example, maybe get them from:
- fish,
- avocados,
- nuts,
- seeds, and
- oils.
The ones that we need to avoid are the trans-fats, “hydrogenated”, “partially hydrogenated”, margarine, or shortenings. These are actually manmade and not found in nature and those foods are not good for organisms.
Another thing to pay attention to is the temperature point where the oil is actually degrading. So if you’re cooking with oil, it’s important you use one that doesn’t degrade at the temperature you’re going to cook.
Coconut oil and olive oil have a higher temperature point. So those are safe for cooking.
PROTEINS
- Produce amino acids (building blocks of neurotransmitters)
- Support growth and repair in the body
- Aim at getting them from a variety of food (animal and/or plant sources). For animal sources, get high-quality ones (e.g. sockeye/red salmon)
- Aim at eating some at each meal incl. breakfast and snacks
Proteins are very important as well. They have less bad press. They produce amino acids, which are the building blocks of neurotransmitters. So they are very important for the brain as well.
They support growth and repair the body.
This means that it’s very important to have protein when we are under stress or to recover from stress, have a high level of exercise, or when we are aging. We need that to grow back and repair the body.
So very important and it’s better to get it from a variety of food as well.
We all know about animal sources of protein including meat, fish, eggs, and dairy.
The important thing is to get high-quality proteins because the lower-quality ones may have some contaminants, toxins, and chemicals.
For fish, for example, it’s important to have those that are less likely to be farmed. Sockeye and red salmon can not be farmed so that would be a better option because it’s less likely to be contaminated.
Plant sources of proteins may be the ones that we know less about. So soy-based like soybeans and soy milk are pretty well known, but also there’s a lot of proteins in quinoa, oats, lentils, nut butter, hemp seeds, and more.
And it’s important to have some in each meal as well, including breakfast and snacks. We’re going to see more why as well later.
CARBOHYDRATES
- Provide energy
- Break down into sugars (glucose and lactose), which support brain function
- Regulate fat metabolism
- Provide prebiotics (from their fibers) that serve as food for probiotics
They also have some bad connotations sometimes.
Carbohydrates are critical because they provide energy and they break down into sugars, which we need to support brain function.
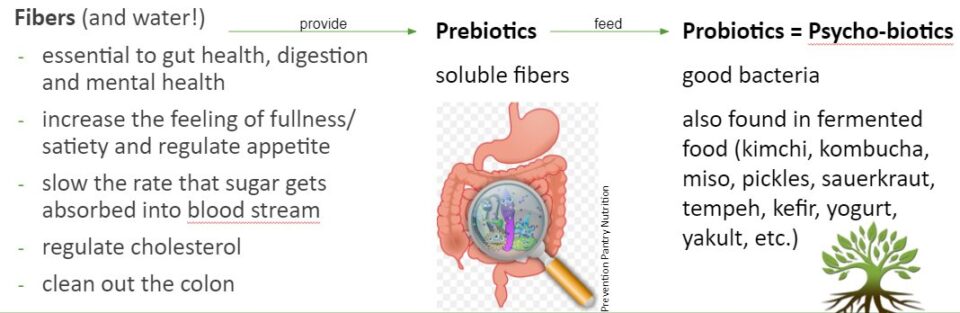
It also regulates fat metabolism and it contains fibers and those fibers are the food for the probiotics. So we’re going to talk about that more info in the next slide.
Let’s see about the mechanism there. So when we eat carbohydrates, if they have fibers, that’s the one we want (we want some with fibers). And if we drink water at the same time as well, this really helps us get healthy proper digestion because the fibers also clean up the colon.
With good digestion comes good mental life as well. They also have a very important role to play in increasing the feeling of fullness/ satiety and regulating appetite. Once your body has the fibers, it feels full so it doesn’t ask you to eat more.
It also slows the rate that sugar gets absorbed into the bloodstream. And it regulates cholesterol. This is because those fibers provide the soluble fibers, which are the prebiotics, which are the food for the probiotics, and the probiotics are really important.
Those fibers are not digestible and that’s why they’re being eliminated, but they are very important.
Probiotics are sometimes actually called psycho biotics because they have such an important role to play in our mental health. Those are good bacteria.
So the prebiotics actually helps feed the probiotics but also put in check so bad bacteria. So it really helps with a balance between the two. It helps the battleground not to proliferate.
Good bacteria are living organisms that support the system. They produce nutrients, like vitamins, and fatty acids (short-chain fatty acids).
And they are also involved in the secretion of neurotransmitters like Gabbar and serotonin. So they’re actually involved in having them help us get those chemicals in balance.
We have them, hopefully, when we are born. But they are affected actually by the type of birth we had. If it was traumatic, that can have affected our probiotics from birth.
Stress also affects probiotics. So it can be important to actually nurse and replenish with probiotics for eating fermented food, for example.
I listed some of them so they are more accessible to you like:
- kimchi,
- kombucha,
- miso,
- pickles,
- sauerkraut,
- tempeh,
- kefir,
- yogurt, and
- yakult.
I know what you would be willing to try, but try and pick one that you feel would be acceptable for your taste.
Stabilization of Blood Sugar is key for mental health and to avoid adrenal exhaustion.
- Aim at getting glucose from fruits and vegetables because:
- They are not as quickly assimilated and calorie-dense as sugars and refined carbohydrates
- They contain fiber which slows the rate that glucose gets absorbed into the bloodstream
- Aim at mixing carbohydrates with high-quality proteins (and fat) because it slows down the uptake of glucose
- Aim at eating when hungry, stopping when comfortably full, which may mean eating more often in smaller quantities
Carbohydrates are involved in blood sugar regulation.
It is very important to regulate the level of blood sugar in the blood because when we are having a high concentration of sugar in our blood, we tend to feel good. We get energized and we have a pretty good feeling.
Sometimes if it gets too high, we get too energized. But when it goes down, we are also affected.
A drop in glucose can cause mood changes like feeling irritable or anxious, having the sensation of fainting, or feeling shaky. Also, craving would appear when the glucose starts to get low, maybe being foggy, confused, inattentive, or having a headache.
A drop in glucose can affect mental health a lot.
So it is important to keep it as stable as possible. How can we do that? And also, what is important is that by having ups and downs, it is the adrenaline that regulates that and it can exhaust the adrenaline system and that can affect their efficiency.
It gets exhausted and is not able to do that regulation.
How can we support that regulation?
Fibers are key because if we eat fibers and that actually slows the rates, that gets absorbed instead of peaking and goes lower. And also, if you eat the carbs mostly from fruits and vegetables, which are not as calorie dense, the sources like sugars or refined carbohydrates are not as quickly assimilated as well. They would get assimilated slowly. So the peak is not going to be as quick and as high.
Another thing that can help is to mix carbohydrates with high-quality proteins and fats, or basically never eat carbohydrates “naked”. Always have carbohydrates with proteins and fat. It’s because cinching helps kind of slow this uptake of glucose.
A way to regulate that is the same as what we said before, is eating when we’re hungry and stopping when we’re full.
That may mean eating more often. And that means that this up and down would be much, much softer, not with such a high amplitude. Since we’re not having these drops, then you won’t feel so hungry.
So it helps to feel full longer as well. That’s the important point.
Fruits, mushrooms, and non-starchy vegetables
Aim at eating a variety of carbohydrates every day, across the color spectrum (green, yellow, orange, red, purple) – each having specific protective properties for the brain and body
- e.g. berries (anti-oxidants), bitter greens (arugula, dandelion, watercress), leafy greens (kale, chard, collards, spinach, etc.), cruciferous (broccoli, cauliflower, Brussels sprouts, etc.)
Carbs are a big category actually.
This includes fruit, mushrooms, and non-starchy vegetables and has a bunch of different categories. That’s why you put them separately.
But what is important there is actually to try to get a variety of them and especially a variety of colors. Somehow the colors can indicate the specific type of protective properties.
So eating fruit and vegetables of different colors has its importance.
- We know that berries, for example, so purple ones and red ones have antioxidants and greens have certain properties as well.
- So we distinguish that bitter greens like arugula, dandelion, and watercress have different properties than…
- leafy greens, which are kale, chard, collards, and spinach.
- Cruciferous vegetables like broccoli, cauliflower, and Brussels sprouts are also a different category.
So try to get a little bit of those throughout your day or your week because they all bring something different to the body and to your brain.
Prefer eating them whole, rather than dried, juiced, or smoothed.
This is because you tend to eat more if they are dried or juice or in smoothies. So you may not realize that you are full before you eat a little bit too much.
Starchy vegetables, legumes, and whole grains
Other types of carbohydrates include starchy vegetables, legumes, or grains.
- Starchy vegetables: potatoes (incl. sweet potatoes), butternut squash, acorn squash
- Legumes: beans, lentils, split peas, nuts, chia seeds, flax seeds, etc.
- Whole grains/cereals: rice, oat/oatmeal, barley, millet, wheat, buckwheat, amaranth, corn, etc.
Have a little bit of a caveat of preferring them whole than floured because flowering tends to break their nutritive properties.
But I mean as everything is just a preference. It is not going to be 100% what we can do there and it doesn’t have to be.
Chronic Inflammation
Chronic inflammation may show as fatigue, obesity, digestive issues, allergies, irritability, bipolar, depression, anxiety, insomnia, chronic pain, or autoimmune disease.
A whole food diet is anti-inflammatory.
- Aim at reducing/avoiding processed food, which have
- Less fibers
- More and lower-quality fats
- Less nutrients, especially less micronutrients (antioxidants, vitamins, minerals, etc.)
- Added salt and sugars
- Added non-food items/toxins (pesticides, fertilizers) / chemicals (e.g. food colorants, additives, preservatives, sweeteners)
I think that’s pretty much it for the carbs, but we cannot finish this chapter before we talk about inflammation and chronic inflammation. So inflammation is actually really needed to recover from the disease. But chronic inflammation is where the problem can lie because it can show us physical issues like chronic pain, autoimmune disease, digestive issues, or allergies, but it can also show us mental health issues.
There is a correlation between depression and chronic inflammation.
So depression, irritability, bipolar, anxiety, and insomnia, all of those have been correlated with chronic inflammation sometimes. So it’s important to make sure that our diet is supporting reducing inflammation in our body.
Unfortunately, drugs are not really a big solution for that. The main thing is actually having a good, healthy diet that would support that. And that tends to be a diet that is more towards whole food than processed food.
The issue with processed food is just that they tend to have less fiber, more and lower-quality fats, and especially to have less nutrients and less micronutrients like antioxidants, vitamins, and minerals. These are barely there in processed food.
They tend to have more salt or sugars and they don’t have things that are not actually food or toxins like pesticides, fertilizers, chemicals like food colorants, additives, preservatives, and sweeteners.
With processed food, we are really increasing the risk of nutrient deficiency. So it’s not just what else we’re getting in our body stuff that may be toxic, but it’s also what we’re not getting in terms of nutrients.
How to improve?
- Add or substitute, rather than take away
- Focus on what you eat on a daily basis, not on occasional treats
- “An imperfect plan done consistently beats a perfect plan done rarely” (Precision Nutrition)
- Use a “dial method” where
- you go from 0 (or current) to 10 progressively – e.g. experimenting for 2 weeks
- you allow yourself to oscillate between 8 and 10 according to circumstances
First, it is important not to focus on what to take away and especially not think:
“Well, I’m not going to eat that flavor now and be very upset about it” because that’s usually not a sustainable way to do things.
So it’s important to think more in terms of what can I actually add that would bring more support to my mental health. Or what can I substitute?
That’s just substituting something that is less healthy for one that is a little bit more healthy. So we’re really thinking more in those terms for making those small adjustments.
And that’s more important to do, like small adjustments than just drastic changes and focusing on what you eat daily, because “An imperfect plan done consistently beats a perfect plan done rarely” (Precision Nutrition).
We need to pay more attention to what we’re doing daily. That’s what really counts most, not what we do once or twice a week or a month. That is not as relevant at all.
Going progressively, maybe thinking more about a continuum from starting at zero to 10 or not processed food at all.
We’re all in continuing there and really going there progressively and more through experimentation of maybe two weeks or a month of changing one thing and see if that works for you.
If it created a challenge then you will have the motivation to continue. And if it didn’t but you have it in your habits now then it’s not a big deal to actually continue it. Well, that’s a win as well.
Also thinking that once you’re up in the levels like maybe 7, or 8, do not think that you have to step at 10 all the time. No, you can also get 6 one day, 9 one day, whatever. It’s not perfection that we’re talking about.
It’s important not to have flexibility without feeling guilty that we’ve not been a 10 today.
That’s not what’s going to make things sustainable and bring a healthier relationship with food and also getting rid of that idea of the willpower thing because it’s about progression.
I mean, when we’re going to be on the hunger scale of like 1 or 2, it’s not going to be about willpower anymore. We’re going to be stressed and we’re going to need to eat right away.
That’s what our body is going to ask and need. So it’s more important to prepare so that in most times where we are, when we are exceptionally up to 1 or 2, we have something healthy ready that we can pick up right away.
That thinking of those investors is much more empowering, that thinking that we always have to have power, which is not the case. We’re going to be stressed.
Beyond Food
Get support from a medical provider to assess for:
- Thyroid issues
- Deficiencies in
- Essential fatty acids (DHA/EPA)
- B-complex vitamins (key for adrenal function and neurotransmitter production, deficiency may show as fatigue, apathy, depression)
- D vitamin (deficiency may show as depression and seasonal affective disorder)
- Magnesium (deficiency may show as hyperarousal like anxiety, muscle spasms, constipation, nerve issues, ADHD)
- Need for adrenal support to restore a healthy HPA axis – may show as feeling alternatively (or at once) wired and tired. Reducing caffeine is key
A little bit of a word about what is beyond food.
We can do a lot through diet, but in some individual cases where we’ve been depleted from those nutrients for so long that we may need a little bit more to do than get them for our diet.
Or there may be some underlying issues that really keep things in balance. This is the part where we may need support from a medical provider.
This could be your functional medicine doctor, naturopath, nutritionist, psychiatrist or dietician, or another medical provider who would be able to assess that for you.
Thyroid issues
One thing to look for is thyroid issues because those can be correlated with mental health issues like depression, for example. So making sure that so far it is functioning properly is very important.
Then, also, maybe assess for deficiencies. Those can be actually assessed by a blood test. For example:
- B-complex vitamins and
- D vitamins can be tested.
- Magnesium is not very reliable.
This (Magnesium tests) is because your body is going to do whatever it takes to keep magnesium in the blood at a proper level. But that may mean that there’s a deficiency somewhere else in the body. So those tests for magnesium may not be as relevant. So watching for the signs is important.
That is why I indicated how it can show. This magnesium deficiency may show as hyperarousal like anxiety, muscle spasms, constipation, nerve issues, and ADHD.
I have not indicated, but it can show as depression, and bipolar psychotic disorders as well. So something to watch for. If that happens to be deficient, then take a high-quality GPA-rich oil, which can be from fish or vegan.
What you need to know about this oil is that it needs to be kept in the fridge. That’s very important. There is always a degradation and I’d better take them with food because that can affect your digestive system.
The B-complex vitamin deficiency can show as fatigue, apathy, and depression because those vitamins are essential for adrenal function, the stress response, and neurotransmitter production.
So if you’re not getting this properly, then that can affect your mental health. That you can be tested for it. You can check your levels and if needed, take a supplementation and just some B-50 complex, for example.
We just need to be careful because you’re going to tend to be energizing since they’re going to combat the depressed or fatigued state. So things I mean, some warnings that it doesn’t interfere with sleep and take them with food as well.
For B-12 specifically, the usual threshold is 200 as a minimum, but for mental health, it needs to be higher. For B-50 it would be more of what we’re looking for as a minimum. So you may want to double-check your tests. And if you’re under 50, it’s actually probably better to supplement B-12 through a supplement or a monthly injection.
D vitamin deficiency can appear as depression or seasonal affective disorder.
It’s pretty common to be D vitamin deficient. It needs to be in the 45-55 range and in increasing that sun exposure helps, but supplementation may help as well. Just be cautious if you have kidney disease for those because that would not be recommended.
For magnesium, it’s difficult to test for it.
Magnesium deficiency may show as a hyperarousal state, like maybe anxiety, muscle spasms, nerve issues, or ADHD.
So anything that is a little bit like keeping you hyper for some time. There’s not really any risk in taking too much apart from if you take too much, you’re going to get diarrhea and a counter indication for people with kidney heart medication.
So just be careful of that if you have that. In any case, ask your provider for any interference with what you’re already taking.
In general, it is advisable to take them and start slow with 100, or 200 mg per day first. And if that doesn’t change much, you can increase. And as I said, your body is going to tell you when it had too much because that’s going to change and turn into diarrhea.
Another thing to know about magnesium is that it’s not absorbed if you’re having too much calcium. So if you’re getting calcium supplementation that can interfere with the magnesium. You may need to lower your calcium intake if you’re actually not needing it so that the magnesium can be absorbed better.
Adrenal support has a big role in the stress support system.
If your adrenal support is not working very well, it could show as feeling alternative (or at once) wired and tired. For that one key aspect is actually to reduce or eliminate caffeine because caffeine artificially tries to support the adrenal, but it doesn’t actually solve the problem.
So actually reducing it so that the adrenal can actually be supported right away. And it can be supported, as we said, by eating regularly, because this way it doesn’t have to take care of your blood sugar all the time, exercising, and managing stress.
B vitamins are important for adrenal support as well. And then you can use specific herbs to support it. And we’re going to not go into too much detail there because you’re going to need support to choose it.
You can have ginseng, ashwagandha, and licorice to help with that. Adrenal is not easy to test either. So that’s kind of the caveat there.
It’s difficult to test if you have a good adrenal system or not.
Ways to stimulate the vagal nerve (parasympathetic nervous system) to enter the “rest and digest” state
- SLEEP
- MINDFUL EATING
- Aim at eating at a table, with others if possible, without distraction. Take a few deep breaths, eat slowly, chew well
- STRESS MANAGEMENT
- Deep breathing, relaxation, mindfulness, mindful movements/exercise, therapy/trauma treatment (since stress/trauma may cause or sustain chronic inflammation)
Another thing beyond food is basically how we are digesting and in which state we are eating because that digestion happens in a state of relaxation. So if you’re stressed or have lack of sleep, that’s going to affect your digestion.
It’s not only about what you eat. You may ingest everything that is healthy, but somehow your digestion doesn’t do its job. So you’re actually not getting the nutrients that you’re supposed to bring in. That the food was actually bringing.
So you may eat perfectly healthy and eat everything that you’re supposed to eat, but then it’s not digested correctly and doesn’t end up being that for yourself and your brain.
So sleep is very important. If you like to sleep you’re going to be much more likely to feel more hungry because it’s going to be that emotional hunger of being fatigued.
You’re going to have more cravings because your body is going to want that energy, that boost. It’s going to crave carbs in particular. So it is very important to get a good amount of sleep.
Eat as much as possible in a state of relaxation so that you can activate your vagal nerve, which is the parasympathetic nervous system, to enter the “rest and digest” state.
That may mean eating at the table rather than on your desk or in your car. Slow down the speed at which you eat, eating and thinking about what you’re eating rather than being distracted by TV or something you’re watching.
Maybe starting with taking a few deep breaths, eating slowly, and chewing well. This is very important because digestion starts with chewing. If it is not chewed well, then the stomach is not going to be able to do the job, and there are going to be residues that are not actually being used.
The importance of stress management is to make that happen so it helps with your breathing, relaxation techniques, mindfulness, mindful movements, and exercise, and if needed, something to be resolved for therapy or trauma treatment because trauma can definitively induce a lot of chronic inflammation.
So having that trauma resolved can help reduce inflammation and reducing overall stress.
References Used
- “Nutritional and integrative medicine for mental health professionals” course by Dr. Leslie Korn
- “Nutritional and integrative interventions for mental health” seminar
- “A therapist’s guide to the psychopharmacology of trauma and dissociation“ webinar by Dr. Frank Anderson
- “Fuel your brain” seminar by Dr. Kristen Allott
- https://ideas-ted-com.cdn.ampproject.org/c/s/ideas.ted.com/a-scientist-explores-the-mysteries-of-the-gut-brain-connection/amp/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5859128/#:~:text=The%20vagus%20nerve%20is%20responsible,%2C%20and%20vomiting%20(17)
- https://www.integrativepro.com/en/articles/the-hpa-axis
- https://www.precisionnutrition.com/blog
I just want to go through the things that I used for this presentation so you can see some names here. Dr. Leslie Korn has books that you can read if you want. Dr. Kristen Allott has presentations available. And those are some of the links to the articles that I used for the research part.
Additional Sources of Information
Where to find:
- Functional medicine doctors (www.ifm.org)
- Naturopaths (www.naturopathic.org)
- Integrative Medicine for Mental Health (https://www.immh.org/)
Where to find nutrition-related resources:
- Dr. Mark Hyman (https://drhyman.com/)
- Dr. Andrew Weil (www.drweil.com)
- Dr. Michael Greger (https://nutritionfacts.org/)
Here are some useful tools to find functional medicine doctors, naturopaths, or doctors for mental health. Also, here are some examples of doctors who are very much in between nutrition and published a lot of resources online. So that can be a good source of information. Dr. Mark Hyman, Dr. Andrew Weil, and Dr. Michael Greger. So just check it out and see if that perhaps provides you with more information.
Eddins Counseling Group provides:
- Individual Health Coaching
- Individual Counseling (for food concerns, anxiety, depression, stress management, trauma treatment, etc.)
- Group Programs:
- Make Peace with Food – Thursdays, online
- Eating Disorder Therapy Group – Wednesday evenings, online
For more information call 832-559-2622, text (832) 699-5001, or email [email protected]
I just wanted to say that we’re offering coaching if that’s of interest to you. We also provide individual counseling for food concerns or other mental health concerns.
We also have some group programs as well, such as Make Peace with Food and Eating Disorder Therapy so that can be done as a group as well.
If you’re interested or if you want to contact us for a 15-minute free consultation to see what your needs may be or answer some questions that you may have, just feel free to reach out at 832-559-2622.
Thank you for watching!